Table of Contents
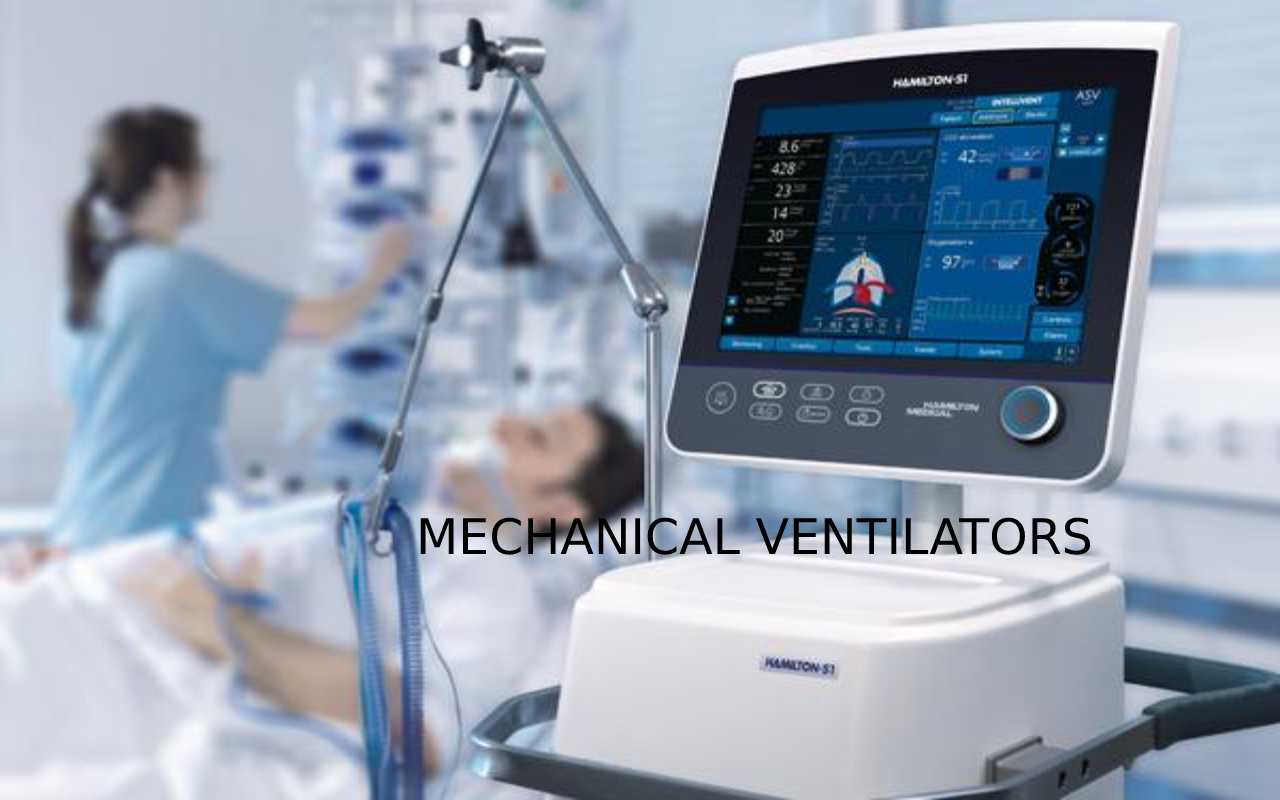
Mechanical Ventilators – Explanation
Mechanical Ventilators if a disorder makes it very difficult for you to breathe or grow sufficient oxygen into your blood. This condition is called respiratory letdown. Mechanical ventilators act as shouts to change the air in and out of your lungs. Your respirational therapist and doctor set the Ventilator to control how often it impulses air into your lungs and how much air you become.
Mechanical VentilatorsYou may be close-fitting with a mask to get air from the Ventilator into your lungs. Or you may feel essential a breathing tube if your breathing problem is more serious.
In mechanical ventilators, existence on a ventilator may make you more liable to pneumonia, damage to your vocal cords, or other problems. Mechanical ventilators are mainly used in infirmaries and transport systems such as ambulances, MEDEVAC air conveyance, etc. In approximate cases, they can be used at home-based if the illness is long term and the caregivers at home obtain training and have good nursing and extra resources in the house.
Travel this Health Topic to learn more about fans, our role in clinical trials, and where to find more information.
Mechanical Ventilators Needs
It may be essential to be on a ventilator aimed at existences, workweeks, or more if you have an injury or illness that makes it hard to breathe.
Some people with COVID-19 have simple difficulty breathing or mature ARDS. However, this only happens in people who become disapprovingly ill, accounting for around 5%Trusted Source of all confirmed COVID-19 cases. In addition, doctors also use ventilators for persons who experience surgery and will not breathe on their own due to anaesthesia.
Doctors sometimes use ventilators for operations because anaesthesia drugs can delay your living. A ventilator may also help you breathe during surgery where you are asleep, but this is usually for a few hours. To place you on a ventilator, your doctor anaesthetizes you. Then, they put a tube unhappy your throat and hook on your windpipe. This makes it calmer to get air into and out of your lungs. The process is called intubation.
Mechanical Ventilators Complications: Infection
The breathing tube in your airway might let in bacteria that infect the tiny air sacs in the walls of your lungs. Plus, the line makes it harder to cough away debris that could annoy your lungs and reason an infection.
This type of infection is called ventilator-associated pneumonia, or VAP. VAP can make it harder to treat your other illness. It’s perilous because you may already be quite sick when you’re put on a ventilator.
Doctors treat it with antibiotics. VAP might need particular types that can fight antibiotic-resistant bacteria in some cases. Even if you already have a contagion, like a viral infection of your lungs, you can get VAP on top of that. Doctors call this a “superinfection.”
Mechanical Ventilators Do and Their Role in COVID-19
A ventilator is a device that chains or re-forms breathing by pumping air into the lungs. Occasionally, people refer to it as a vent or breathing machine. Doctors use ventilators if a being cannot live adequately on its own. This may be because they undergo general anaesthesia or have an illness that affects their breathing.
Ventilators play an essential role in saving lives in hospitals and ambulances. There are different Ventilators, and each offers varying levels of provision—the type of doctor usage will depend on a person’s condition. Persons who require long-term ventilation can also use them at home.
Types of Ventilators
There are several ways a being can receive ventilator support. These include:
Face mask ventilators
Mechanical ventilators
Manual resuscitator bags
Tracheostomy ventilators
Face mask ventilators are non-invasive, while mechanical and tracheostomy ventilators are offensive and work via tubes that a doctor supplements through a hole in the neck that leads to the trachea or windpipe. Healthcare experts’ term this intubation.
People who physically struggle to respire self-sufficiently may require mechanical ventilation. A face mask ventilator might be enough to steady their disorder for some. Below, we look at the respective type of Ventilators and how that.
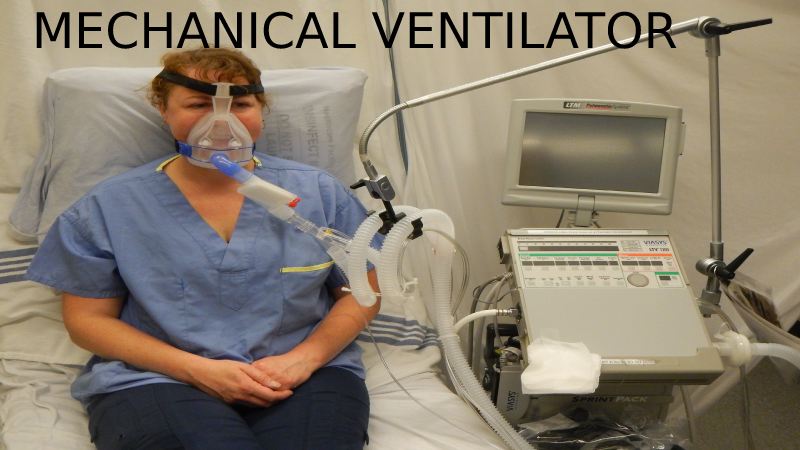
Mechanical Ventilators of Face Mask
A face mask ventilator is a non-invasive technique of supportive breathing and oxygen levels. To use one, a person attires a mask that fits over the nose and mouth while air blows into their airways and lungs.
People with COVID-19 may use a face mask ventilator if they have difficulty breathing or do not have sufficient oxygen levels. Continuous positive airway pressure (CPAP) and bi-level confident airway heaviness (BiPAP) devices also operate via a face cover.
People often use these for stable conditions, such as chronic unhelpful pulmonic disease, but some doctors may also use them for persons with COVID-19.
In addition to secondary oxygen levels, PAP therapy can also aid in expelling carbon dioxide levels. Whether a doctor chooses to use CPAP or BiPAP will depend on a being’s original condition.
Mechanical Ventilators
Mechanical ventilators are machines that take end the prearranged procedure. Doctors custom these when a person cannot breathe on their own.
Mechanical ventilators effort via a tube in a person’s throat, driving air into the lungs and also removing carbon dioxide.
A ventilator unit orders the pressure, humidity, volume, and also air temperature, relying on a doctor or respiratory therapists controls. This allows healthcare professionals to switch a person’s living and also oxygen levels.
People with COVID-19 may need a powered ventilator if they are disapprovingly ill.
Manual Resuscitator Bags
Manual resuscitator bags are pieces of apparatus that allow people to control the airflow of their Ventilator with their hands. These plans consist of an empty bag, or “bladder,” that a person crushes to pump air into the lungs.
A person can confer one of these devices to a face mask ventilator. If they are intubated, a medic can attach one to the tube in their throat.
This can be useful as a quick answer if a being on a mechanical ventilator needs to stop using it. For example, if there is a controlled outage. A person can use a manual resuscitator bag to come aimed at the influence to come back on.
Tracheostomy Ventilators
Individuals who have felt a tracheostomy will need a ventilator.
A tracheostomy is a procedure anywhere a doctor makes an opening in the windpipe and inserts a pipe, allowing air to flow in and also out. This allows a person to breathe without using their nose or mouth.
In its place of inserting a ventilator through the mouth, doctors pull out it directly into the windpipe. People who suffer tracheostomies can and also receive a ventilator. Support through this opening. People may require tracheostomies if they need motorized ventilation for an extended time and also need more time for rehabilitation.
Others may require long-term tracheostomies. If they have conditions such as chronic lung disease or a neuromuscular disorder that weakens the breathing muscles. Some individuals can manage their tracheostomy at home-based.
Risks of using ventilators
As with many medical procedures, the ventilation includes some risks, mainly mechanical ventilation. The lengthier a person requires mechanical ventilation, the advanced the stakes.
Potential complications of using a ventilator.
Atelectasis occurs when the lungs do not expand fully, but dropping the quantity of oxygen that arrives in the bloodstream
Aspiration, or breathing matters or fluids, but such as saliva, into the airlines
lung damage, which can outcome from high air pressure or high oxygen levels
pulmonary oedema, which occurs when fluid shapes up inside the airbags in the lungs
pneumothorax, which happens when air is holey from the lungs into the planetary just external of them, causing pain, shortness of breath, and also — in some cases — whole lung collapse
infections, which can include sinus infections
Airway obstruction
Long-term vocal cord injury as a result of intubation
Blood clots or sores as a result of lying in one position extend areas
Muscle faintness, if a person stays on a ventilator for an extended period
Delirium, which can become principal to psychological trauma or post-traumatic pressure complaint
Healthcare workers giving people with COVID-19 have an increased risk Trusted Source of coming into contact with the SARS-CoV-2 virus, which reasons the disease, during intubation. Doctors and also nurses can take ladders to reduce the likelihood of these complications.
Mechanical Ventilators the Steps
They closely monitor people on ventilators for signs of complications, adjusting the air pressure and oxygen levels to match a patient’s normal levels and wearing personal protective equipment to protect against viruses and prevent their spread to others. Treating bacterial infections with antibiotics. Ensuring patients receive physical and pulmonary restoration after they leave ICU
Conclusion
Ventilators are devices that support a person’s living if they are feeling a respiratory failure.
There are different types of Ventilator, including non-invasive and invasive, that deliver variable degrees of sustenance. Demand for ventilators increases due to COVID-19.
Serious illness can influence physical and mental health. People experiencing tenacious symptoms after weaning off ventilator support must seek guidance from a doctor. It can take time to recuperate from being on a ventilator.